Covid ‘Vaccination’ Linked to 6,800% Higher Odds of Debilitating Autoimmune Muscle Disease

CDC/FDA data reveal a massive safety signal for polymyalgia rheumatica—an autoimmune inflammatory disease causing severe muscle pain and debilitating stiffness.
A new study titled “Association Between COVID-19 Vaccination and Polymyalgia Rheumatica: A Review and Case Series Report” reports a powerful safety signal linking COVID-19 vaccination to polymyalgia rheumatica (PMR)—a debilitating autoimmune inflammatory disorder characterized by severe muscle pain and systemic inflammation.
The paper was authored by Dr. Erik Nilssen, Dr. James Thorp, Claire Rogers, Kirstin Cosgrove, Dr. Steven Hatfill, Dr. Drew Pinsky, Dr. Kelly Victory, Dr. Alejandro Diaz-Villalobos, Nicolas Hulscher (myself), and Dr. Peter A. McCullough.
In our analysis, we examined reports from the CDC/FDA Vaccine Adverse Event Reporting System (VAERS) and detected a striking disproportionate increase in PMR cases following COVID-19 vaccination compared with other vaccines. We also report three clinical cases of polymyalgia rheumatica observed in recent medical practice following COVID-19 vaccination or spike protein exposure.
Polymyalgia rheumatica primarily affects adults over age 50 and can leave patients with crippling shoulder, neck, and hip pain, profound morning stiffness, fatigue, and elevated inflammatory markers. Many patients require long-term corticosteroid therapy to control symptoms.
Massive Safety Signal Detected in U.S. Vaccine Database
We analyzed reports from the CDC/FDA Vaccine Adverse Event Reporting System (VAERS) spanning 1990–2026 and identified:
- 2,227 cases of polymyalgia rheumatica reported after COVID-19 vaccination
- 233 cases after influenza vaccination
- 526 cases after all other vaccines combined
After adjusting for the duration of vaccine availability, the safety signal became striking.
The odds ratio over time (ORt) for PMR following COVID-19 vaccination compared with influenza vaccination was:
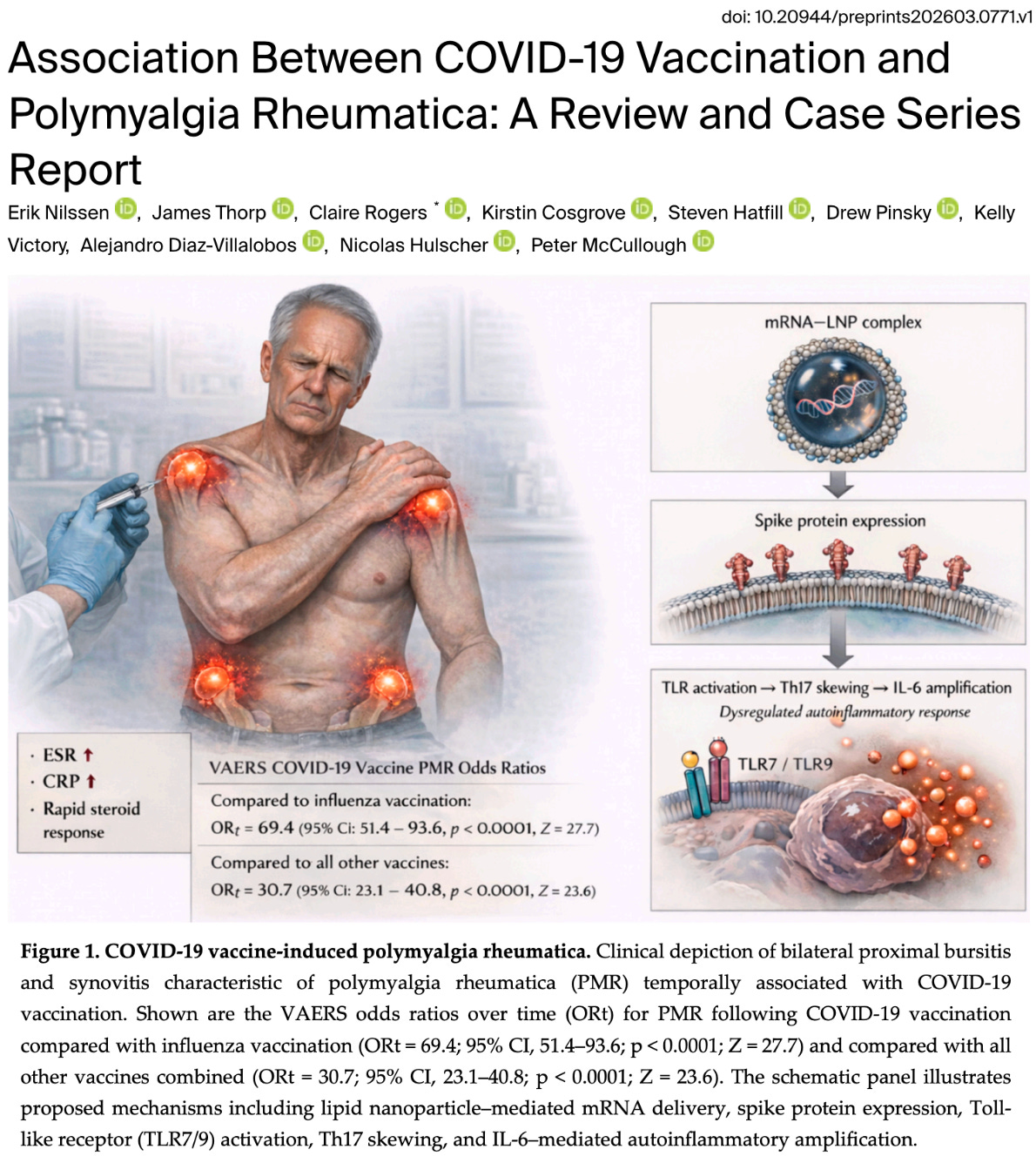
69.4 (95% CI: 51.4–93.6, p < 0.0001, Z = 27.7)
When COVID-19 vaccination was compared with all other vaccines combined, a similarly strong signal persisted:
30.7 (95% CI: 23.1–40.8, p < 0.0001, Z = 23.6)
For context, regulators define a vaccine safety signal as a disproportionality measure of ≥2.
These findings exceed that threshold by more than an order of magnitude, indicating an unusually strong association between COVID-19 vaccination and reports of polymyalgia rheumatica.
The extremely large Z-scores—23 to 27 standard deviations above expected values—indicate that the probability of this signal occurring by chance is extraordinarily small.
Real-World Clinical Cases
In addition to the database analysis, we describe three clinical cases observed in clinical practice.
Case 1
A previously healthy 51-year-old physician developed severe PMR with elevated inflammatory markers and extremely high spike antibody levels exceeding 21,000 U/mL.
Case 2
A 65-year-old man developed debilitating shoulder and hip pain after receiving two Pfizer COVID-19 vaccine doses. He required prolonged steroid therapy.
Case 3
A 59-year-old physician developed PMR two weeks after his second vaccine dose, requiring years of treatment before remission.
Spike Protein May Trigger Autoimmune Inflammation
We propose that spike protein exposure may initiate autoimmune pathways capable of producing inflammatory musculoskeletal disease. Possible mechanisms include:
- Molecular mimicry between spike protein and human tissue
- Activation of Toll-like receptors (TLR7 and TLR9)
- Th17 immune activation
- IL-6 driven inflammatory cascades
These immune disruptions can lead to bursitis, synovitis, and systemic inflammation characteristic of polymyalgia rheumatica.
Polymyalgia rheumatica is not a minor side effect. Patients may experience:
- severe muscle pain and stiffness
- systemic inflammation
- chronic fatigue
- long-term steroid dependence
- relapses lasting years
Because PMR primarily affects older adults, it may be misattributed to aging or degenerative disease, potentially masking vaccine-related triggers.
Our findings underscore the need for heightened clinical awareness of polymyalgia rheumatica following COVID-19 vaccination and for future research to prioritize direct detection of spike protein and improved monitoring of musculoskeletal complications.
https://www.thefocalpoints.com/p/breaking-study-covid-19-vaccination
